Depression Findings Among Adults in the United States, 2019
Key CDC depression statistics findings
Data sourced from the National Health Interview Survey conducted by the CDC
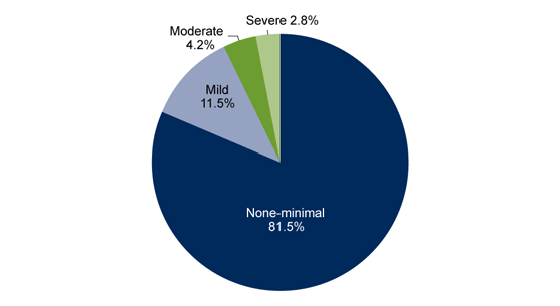
In 2019, 18.5% of adults had depression symptoms.
- Among adults, 11.5% felt mild symptoms of depression, 4.2% experienced moderate symptoms, and 2.8% experienced intense symptoms.
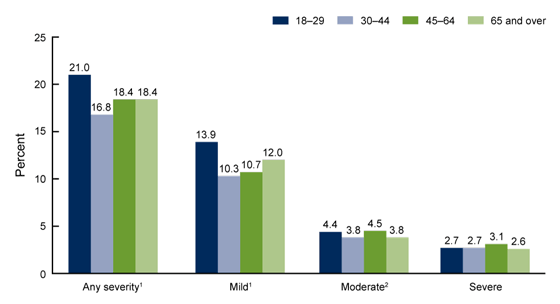
- The percentage of adults who felt any signs of depression was the most among adults age 18 to 29 (21.0%), followed by adults age 45 to 64 (18.4%) and 65 and over (18.4%), and finally the smallest groupd were adults age 30 to 44 (16.8%).
- Women were much more likely vs. men to feel mild, moderate, or intensive symptoms of depression.
- Non-Hispanic Asian adults were less likely to experience mild, moderate, or severe symptoms of depression compared with Hispanic, non-Hispanic white, and non-Hispanic black adults.
Depression is defined by the existence of emotions of sadness, emptiness, or irritability, along with physical and cognitive developments lasting at least two weeks that substantially impact a person’s ability to function (1).
Subject matter: depressive disorder, mental health, depression statics.
Why Depression is at an all time high Now?
The number of people reporting signs of anxiety and depression since the start of the pandemic hit an all-time high in September 2020, just over a year ago. As the pandemic relentlessly persists, we are seeing the highest levels of anxiety and depression reported since the pandemic hit the U.S. last year.
Other Significant Risk factors for depression include:
- Experiencing traumatic or stressful events, such as physical or sexual abuse, the death of a loved one, or financial problems
- Going through a major life change‚ even if it was planned
- Having a medical problem, such as cancer, stroke, or chronic pain
- Taking certain medications
- Using alcohol or drugs
- Having blood relatives who have had depression
Symptoms
The Centers for Disease Control and Prevention (CDC) has recognized that having certain mental disorders, including depression and schizophrenia, can make people more likely to get severely ill from COVID-19.
If you have been experiencing some of the following signs and symptoms most of the day, nearly every day, for at least two weeks, you may be suffering from depression:
- Persistent sad, anxious, or “empty” mood
- Feelings of hopelessness, or pessimism
- Irritability
- Feelings of guilt, worthlessness, or helplessness
- Loss of interest or pleasure in hobbies and activities
- Decreased energy or fatigue
- Moving or talking more slowly
- Feeling restless or having trouble sitting still
- Difficulty concentrating, remembering, or making decisions
- Difficulty sleeping, early-morning awakening, or oversleeping
- Appetite and/or weight changes
- Thoughts of death or suicide, or suicide attempts
- Aches or pains, headaches, cramps, or digestive problems without a clear physical cause and/or that do not ease even with treatment
Not everyone who is depressed experiences every symptom. Some people experience only a few symptoms while others may experience many. Several persistent symptoms in addition to low mood are required for a diagnosis of major depression, but people with only a few – but distressing – symptoms may benefit from treatment of their “subsyndromal” depression. The severity and frequency of symptoms and how long they last will vary depending on the individual and his or her particular illness. Symptoms may also vary depending on the stage of the illness. [1]
Anxiety at an All Time High
The pandemic has forced some people to work and expose themselves to the virus, while others have benefited from working from home.

Google searches for anxiety symptoms from mid-March to mid-May were the highest they’ve been in the history of the search engine, according to researchers at the Qualcomm Institute’s Center for Data-Driven Health at the University of California San Diego. [2]
At the start of the pandemic, some people enjoyed more relaxed lockdown measures (depending on which country they were in), while others felt safer through strict self-isolation.
Still, overall, the mental effects of lockdown did not fail to appear: People reported feeling more agitated, more stressed, more restless, and more sleepless.
This surge in depression and anxiety, while worrying, is not surprising given the numerous challenges the pandemic has posed to so many of us.
Emotional signs of a panic attack include symptoms such as feeling tense or nervous, worrying about the past or future, feeling tearful, and not being able to sleep or relax.
If you’re experiencing panic attack symptoms, medical experts recommend calm breathing practices, getting enough exercise, eating a healthy diet, seeking out peer support, and seeking professional help.
Mental health experts also say that it can be useful to practice gratitude and establish a schedule. Especially during the coronavirus crisis, it’s important to be careful with how and when you engage with the media if the news is driving your anxiety. And limiting social media use can help too, as they can spread misinformation and conspiracy theories about the virus.
Symptoms

Physical Symptoms
Some of the physical symptoms your loved one may report feeling include:
- Lightheadedness
- Sweating
- Nausea
- Feeling edgy and/or restless
- Shortness of breath
- Diarrhea
- Getting easily fatigued
Anxious Thoughts
People with anxiety often have thought patterns such as:
- Believing the worst will happen
- Persistent worry
- All-or-nothing thinking
- Overgeneralizing (making overall assumptions based on a single event)
Anxious Behaviors
Perhaps what you’ll notice most are your loved one’s behaviors. [3] Common anxiety behaviors include:
- Avoidance of feared situations or events
- Seeking reassurance
- Second-guessing
- Irritability and frustration in feared situations
- Compulsive actions (like washing hands over and over)

Covid-19 Depression
The COVID-19 Pandemic has added to increased feelings of isolation and vulnerability to many individuals. There are increasingly severe detrimental consequences of the present pandemic on general mental health; including deterioration of existing issues such as contagion fear, anxiety, social isolation, and chronic stress.
The Centers for Disease Control & Prevention, the Substance Abuse & Mental Health Services Administration (SAMHSA) and the U.S. Department of Education collected data between 2017 and 2018 (pre-pandemic). Key findings [4] show that the nation was ill-prepared from the start to tackle the mental health effects of the pandemic, with worsening mental health leading up to it:
- Nationwide, almost one in five people (47.1 million) in the U.S. are living with a mental health condition. That number increased by about 1.5 million over last year’s report.
- About 10% of youth in the U.S have severe depression. This was highest among youth who identify as more than one race, at 12%.
- Overall, 57% of adults with a mental illness receive no treatment and 60% of youth with depression do not receive any mental health treatment.
- Utah ranked last in overall adult mental health, and Hawaii ranked first.
- About 8% of people in the U.S. struggle with a substance abuse disorder. The District of Columbia had the highest rates of adult substance abuse disorders (13%), with Texas ranking lowest at 6.3%.
- Just under 11 million people had serious thoughts of suicide, and that number increased by 460,000 from the previous year. Utah ranked last, with the highest percentage of adults with suicidal thoughts, while New Jersey ranked first with the lowest percentage.
- Just under 11% of people in the U.S. with a mental illness are uninsured. This increased for the first time since the Affordable Care Act passed and they are the first numbers to reflect the Trump administration’s impact.
Coping with All Time High Depression Incidents
The COVID-19 pandemic has had a major effect on our lives. Many of us are facing challenges that can be stressful, overwhelming, and cause strong emotions in adults and children. Public health actions, such as social distancing, are necessary to reduce the spread of COVID-19, but they can make us feel isolated and lonely and can increase stress, depression, and anxiety. Learning to cope with stress in a healthy way will make you, the people you care about, and those around you become more resilient.
Stress, anxiety, depression can cause the following:
- Feelings of fear, anger, sadness, worry, numbness, or frustration
- Changes in appetite, energy, desires, and interests
- Difficulty concentrating and making decisions
- Difficulty sleeping or nightmares
- Physical reactions, such as headaches, body pains, stomach problems, and skin rashes
- Worsening of chronic health problems
- Worsening of mental health conditions
- Increased use of tobacco, alcohol, and other substances
It is natural to feel stress, anxiety, grief, and worry during the COVID-19 pandemic. Below are ways that you can help yourself, others, and your community manage stress.
Healthy Ways to Cope with Stress, Anxiety, Depression
Here are some tips to cope with daily pressure and depression in these challenging times [5] according to CDC:
- Take breaks from watching, reading, or listening to news stories, including those on social media. It’s good to be informed but hearing about the pandemic constantly can be upsetting. Consider limiting news to just a couple times a day and disconnecting from phone, tv, and computer screens for a while.
- Take care of your body
- Take deep breaths, stretch, or meditate
- Try to eat healthy, well-balanced meals
- Exercise regularly
- Get plenty of sleep
- Avoid excessive alcohol, tobacco, and substance use
- Continue with routine preventive measures (such as vaccinations, cancer screenings, etc.) as recommended by your healthcare provider
- Get vaccinated with a COVID-19 vaccine
- Make time to unwind — Try to do some other activities you enjoy
- Connect with others — Talk with people you trust about your concerns and how you are feeling
- Connect with your community- or faith-based organizations — While social distancing measures are in place, try connecting online, through social media, or by phone or mail
Tips that Work to Help Someone Having Anxiety and Depression at an All Time High
Typical responses to someone with anxiety are often unhelpful. Here are actions you should avoid and what you can do suggested by Johns Hopkins Medicine:
1. Don’t Enable
It’s common to want to help your loved one avoid painful situations by going out of your way to eliminate the cause for concern.

Avoiding difficult situations doesn’t give your loved one the opportunity to overcome fears and learn how to master anxiety. Instead, it makes their world smaller as what they can do becomes more and more limited by their growing anxiety.
2. Don’t Force Confrontation
On the other hand, it’s also not good to force a person to do something they’re scared of. Learning how to overcome deep apprehension is work best done in partnership with a professional therapist. This takes the burden off you. It also empowers your loved ones by helping them face their fears one step at a time with guidance from somebody with experience.
3. Provide Validation
Many different things can make people anxious. Ask your loved one how you can provide support during challenging moments.
4. Express Concern
When you start to notice your loved one withdrawing from activities that they used to enjoy, you don’t have to cover up your concern. Instead, it can be helpful to approach your loved one in a warm and positive way. Depending on how the conversation goes, you might ask if they think they need some help or support in coping with their anxiety.

Taking care of yourself can better equip you to take care of others. During times of social distancing, it is especially important to stay connected with your friends and family. Helping others cope with stress through phone calls or video chats can help you and your loved ones feel less lonely or isolated.
Encourage a loved one who’s struggling with stress, anxiety, and depression at an all time high to make an appointment with a mental health provider. Whenever you need someone to talk to about treatment options to suit your situation, contact us here at We Level Up. Even if we can’t help you, we’ll guide you to where you can get help. There’s never any obligation.
Sources:
[1] Products – Data Briefs – Number 379 – September 2020 (cdc.gov) Depression – National Institute of Mental Health
[2] https://jamanetwork.com/journals/jamainternalmedicine/fullarticle/2769543?guestAccessKey=9f557333-9775-4de7-a640-4cd9ed0d985b&utm_source=For_The_Media&utm_medium=referral&utm_campaign=ftm_links&utm_content=tfl&utm_term=082420
[3] How to Help Someone with Anxiety – Johns Hopkins Medicine
[4] https://www.globenewswire.com/en/news-release/2020/10/20/2111263/0/en/Number-of-people-reporting-anxiety-and-depression-nationwide-since-start-of-pandemic-hit-all-time-high-in-September-hitting-young-people-hardest.html
[5] Coping with Stress – Centers for Disease Control and Prevention